Closing RCM Gaps with Next-Gen Laboratory Billing Solutions

Need a custom demo?
Use your own workflow and see where DocKnow can reduce manual work.
Get your demoLaboratories are dealing with a lot of denied claims, and there’s not one root cause. It’s a combination of issues like outdated laboratory billing solutions, compliance blind spots, and bad data.
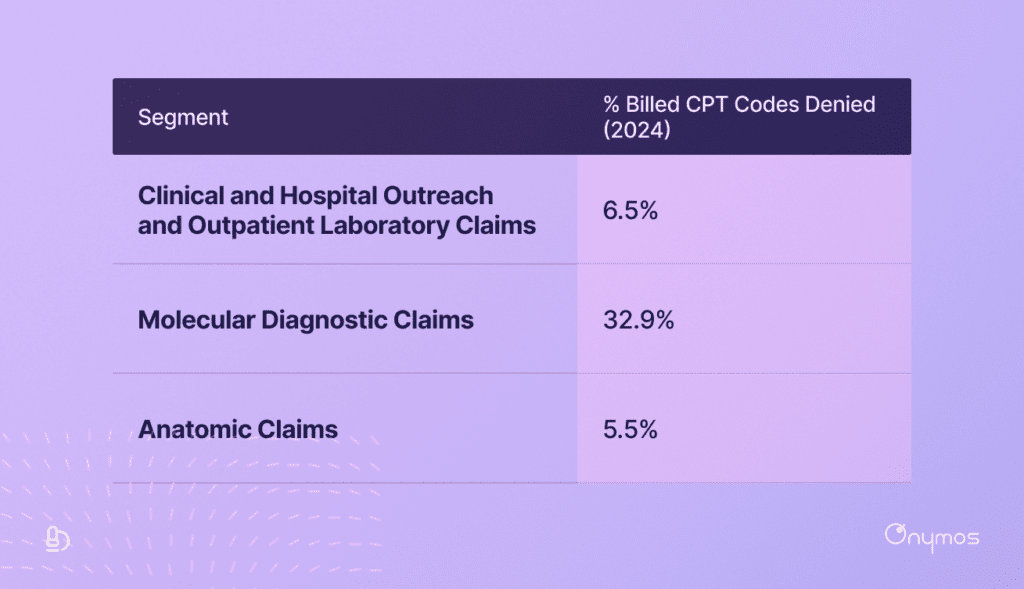
Molecular diagnostics has it the worst. For those claims, denial rates are above 32%. RCM teams just can’t work them all. It’s why some laboratories are actually writing off as much as 20% of their earned revenue.
Tony Mancuso, Director of Innovations at Onymos, says, “It is a huge problem for laboratory revenue cycle management, and it doesn’t help that a lot of labs are short-staffed, and they don’t have the bandwidth to manage all of the eligibility checks and prior auths for the volume of claims they’re processing.”
All of this is why a new class of purpose-built technology is emerging, focused on solving upstream workflow challenges that traditional billing software doesn’t (and can’t) address.
Onymos DocKnow validates data at the first touchpoint
The billing process starts at intake. When coding errors, missing documentation, or mismatched data aren’t detected upfront, claims fail downstream. Labs will only discover problems after a denial arrives, weeks later, when recovery is slower and more expensive (or outright impossible).
For these labs, revenue loss is reactive instead of preventable.
DocKnow’s foundation has always been data reconciliation at scale, but our team continues to innovate how data is captured, validated, and analyzed across every laboratory workflow. Today, DocKnow users can automate eligibility checks at the point of intake, instantly generate appeal packets for payers when denials do happen, and much more.
R1’s specialized LLMs optimize payments
One of the biggest sources of revenue leakage in laboratory billing isn’t denied claims themselves. It’s failing to fully understand how payer contracts determine reimbursement in the first place.
Trying to prevent these kinds of losses isn’t just “time-consuming,” it requires specialized expertise in payer contracts and financial modeling.
Or, it did. Until R1 teamed up with Palantir last year to create R37, an applied AI lab for building new technologies that are deployed directly into R1’s RCM solutions. Its “next-generation payer contract analysis” research is finding ways to automate contract analysis for maximizing payments with LLMs.
Waystar’s AltitudePredict transforms claims forecasting
Finding patterns in denials is retrospective by nature. Combined with constantly changing payer requirements and evolving laboratory compliance standards, implementing and maintaining process improvements isn’t easy. That’s why Waystar is developing an AI to surface risk identification pre-postmortem.
By applying predictive models to claim data, payer behavior, and reimbursement trends, AltitudePredict helps laboratories identify high-risk claims and potential delays in real time.
Redox interoperability closes the loop
Even when claims are correct and approved, revenue can still slow down or get lost in the handoffs between billing systems, payment gateways, and CRMs.
Redox specializes in closing those gaps by ensuring healthcare systems can reliably exchange and interpret data. When information changes in one system (such as a claim status update or payment confirmation), Redox routes and translates that data so downstream systems stay aligned.
It provides standardized integrations with major healthcare platforms and APIs, helping organizations connect EHRs, billing systems, and third-party tools without building custom integrations for each one.
The future of laboratory billing is layered, intelligent, and proactive
Laboratories don’t lose revenue in one place.
Preventing that revenue loss means rethinking the processes around the entire lifecycle of a claim, not just at the claim submission itself.
In the short term, solutions like these will be a competitive advantage for the labs that implement them and treat lab billing holistically. In the long-term, they’ll be operational table stakes.
If your team is evaluating ways to close revenue gaps, the Onymos team can help you assess where automation and intelligent document processing can have the biggest impacts.
Connect with our team to explore how Onymos solutions can maximize efficiency, minimize costs, and drive real, scalable growth.
Schedule your demoWe know healthcare data
AI in the lab. Workflow automation at scale. Digital front doors for hospitals and clinics. Healthcare and life sciences are changing fast. Are you ready? Subscribe to our blog for:
- Trends in healthcare tech
- Research and analysis
- Customer stories and more
